There is lots of interesting news about hot health start-ups like Theranos, Amino, and 23andme, any of which deserves a post (and may yet get one), but I find myself thinking about battleships...and robots.
I've had in mind a post comparing hospitals to battleships. Battleships were once the crown jewel of navies, massive and full of firepower, but which now are at best only museum pieces. A conventional wisdom is that battleships grew obsolete due to higher tech innovations like aircraft carriers and guided missiles. I recently read an analysis that brought up another factor that led to their demise: labor costs. They're just incredibly expensive to staff.
Just like hospitals, or nursing homes.
Consider the results of a new study on health care spending. It retrospectively looked at spending for Medicare beneficiaries who died between 2005 and 2010. The most expensive cohort? Patients with dementia. Not heart disease, not cancer, not other conditions, but dementia. And not by a little; they spent more than 50% higher than the other cohorts, averaging some $287,000.
It gets worse. Medicare spending was actually fairly similar across all cohorts, but out-of-pocket spending was much higher for the dementia patients, leading to the higher overall spending. They're not racking up huge bills getting invasive surgeries or expensive chemotherapy. They're not taking advantage of all these slick new machines in these beautiful new hospital additions. Instead, they're spending time -- lots of time -- getting care in nursing homes or at home.
If they're lucky, they may qualify for Medicaid, which may help pick up some of these costs for custodial care, as it is not typically covered by Medicare. Of course, that's a strange kind of lucky, because it means they've spent virtually all their assets in order to qualify.
Well, at least they get the care they need, right? Unfortunately, many people with dementia, or with other long term disabilities, spend too much time waiting for care. Not so much medical care as help with things most of us take for granted -- getting in and out of bed, going to the bathroom, taking a shower, even eating. Go into a nursing home or assisted living facility and it won't take too long to find residents who are waiting -- knowingly or not -- for assistance with those kinds of tasks.
It doesn't help that there is already a labor shortage for the kind of workers who provide such care, whether in institutions or at home, and that shortage is predicted to grow. The field already has an older workforce, it is a very demanding job, and the pay is low. No wonder turnover in nursing homes averages over 50%. Last year The Wall Street Journal estimated that the need for health care aides will increase by 48% from 2010 to 2020. And 2020 is nowhere near the peak of the baby boomers aging, so the need for these workers will keep growing. It's a recipe for disaster.
Enter the robots.
There are already robots in health care. Robotic surgery, delivery robots, robotic prescription dispensing systems, even therapeutic robots used in lieu of pet therapy But we've just scratched the surface, because we still think of care as being something that is delivered by a person.
People like to talk about the importance of the human touch, but when it comes to something like getting out of bed when I want to, I think I'd rather have immediate service from a robot than an indeterminate wait for help from an aide. And there are some more unpleasant tasks -- like assistance with going to the bathroom -- where I'd prefer not to have to ask another person to help me at all. Sometimes impersonal is better (just be gentle, please).
A 2012 Georgia Institute of Technology survey found that even the current generation of seniors was surprisingly open to having robots help them with household tasks, although they tended to still prefer humans for personal care. The respondents were healthy and independent, and I wonder how much more open they'd be to robotic help for personal care as well if they'd had more experience with receiving such care from health aides.
I also wonder how their children might have responded, if it came to a decision about using robot aides for their parents versus putting them in a nursing home, paying for home care, or providing it themselves.
A follow-up survey of healthcare workers found them also receptive to assistance from robotic helpers -- even preferring them to humans for some tasks, like transferring, medication reminders, or taking vitals. As one of the lead researchers said: "In fact, the professional caregivers we interviewed viewed robots as a
way to improve their jobs and the care they’re able to give patients."
The robots are ready, or nearly so. I've previously written about Toyota's Partner Robot Family. Toyota announced in July that they were putting the home helper robot R&D in "high gear," specifically citing the goal of assisting independent living for the elderly and disabled. Japan is also the home of Robear, which is billed as an experimental nursing-care robot. Robear can already assist with transfers, and the leader of its development team said: "We really hope that this robot will lead to advances in nursing care, relieving the burden on care-givers today."
Japan is a natural locus for these efforts, as it has both expertise in manufacturing -- which has already been revolutionized by robots -- and has one of the oldest and most rapidly aging populations. When the care shortage hits, it is going to hit first in Japan.
We really don't have a lot of options. We can come up with cures that prevent people from getting conditions that rob them of their independence. We can throw more people at the problem, if we can find the money -- or the people. Or we can use technology to help, and that probably means some kind of robots.
The first two options might be nice, but I think we better be getting the robots ready.
I may not live long enough to see artificial intelligence serving directly as a clinician, as I've previously written about, sorry to say. But a personal care robot to help us to stay independent, or at least less dependent on health aides? That's something that we should be able to do sooner rather than later.
OK, iRobot -- maybe spend more time on this and less time on building a better Roomba.
Writing about things that interest me, usually related to healthcare, technology, or innovation. No idea is sacred.
Wednesday, October 28, 2015
Wednesday, October 21, 2015
I'm Shocked, Shocked
Some new research on the effect of physician practice arrangement has on spending offer some disappointing -- but not entirely surprising -- results.
Take physician groups. The death of the independent physician practice, working solo or in a small practice, has long been predicted (and nostalgically lamented). Honestly: would you rather be treated by a doctor practicing alone, or by one at the Mayo Clinic? Physician groups allow for things like development of best practices, administrative efficiencies, and, in this era of Big Data, larger data sets that can be used to improve patient care. When it comes to physician groups, bigger would seem to be better.
If physician groups are good, the theory goes, then integrating them clinically and financially with hospitals, such as through partnerships or common ownership, should even better. That allows for more aligned incentives and better coordination across the continuum of care. Everyone loves Kaiser-Permanente, right?
The AMA says solo practice physicians now are only 17% of all physicians, down from 40% in 1983, and that physician ownership of their practice has declined from 76% in 1983 to just over 50% now (although other surveys say as few as 35% of physicians described themselves as independent practice owners, down from 62% as recently as 2008). Our health care system, it would seem, is destined to be made up of large physician groups, many of which will be owned by hospitals.
Too bad both larger groups and hospital ownership apparently end up costing us more.
A new study in Health Affairs found that as physicians concentrate in larger groups, prices tend to go up, at least for the 15 high volume, high cost procedures the authors looked at. Twelve of the 15 procedures had prices that were 8 to 26 percent higher in areas with the highest physician concentrations; they found no significant relationship for the remaining three.
It might seem that whatever savings might be gained by becoming part of a group are not being passed on to consumers (or their health plans), and/or larger size allows groups to bargain for better reimbursement rates from payors.
An earlier survey, by one of the lead authors of the new study, found that more competition among physicians did, in fact, result in lower prices, at least for office visits. One might conclude that more concentration into larger physician practices may have less to do with greater efficiency or higher quality than it does with reducing competition.
The moral appears to be, if you don't want to compete with them, join them!
Then there is the hospital ownership effect. A study in JAMA Internal Medicine found that increased hospital/physician financial integration led to greater spending, primarily in outpatient care and almost entirely due to higher prices, not higher utilization. Again, the price increases are attributed to greater bargaining power. As one of the authors told The Wall Street Journal: "The market power that is in the hospital’s hands is conferred to the physician practice."
The AHA protests that the study "is not reflective of the changes happening in today’s health-care market," citing newer value-based payment arrangements and hospital price increases that are at historically low levels. That's kind of like saying, well, we weren't taking advantage of you before, but -- trust us -- in the future we really won't take advantage of you.
One visible impact of hospital ownership on physicians is the infamous facility fee add-on. You've been going to the same doctor for years, then the practice gets bought by a hospital, and the next time you go your bill suddenly has this "facility fee" added onto it. Same services, same office, same doctor -- but more expensive.
A good example of this practice is in Pittsburgh, where Highmark unilaterally decided to stop paying such fees for chemotherapy done at UPMC-owned oncologists' offices. Highmark says the fees are "irrational." UPMC says they are not only necessary but standard practice, including at Highmark's own hospital system, Allegheny Health. The matter is in court.
These kinds of fees, based on "place of service," are expressly permitted by Medicare, although one has to assume that they were not the intent of those rules. Of course the AHA defends them, saying that hospital-owned practices can bill as an outpatient facility because they are subject to the more onerous requirements that other hospital outpatient services are, but they just don't pass the sniff test. That's not supposed to be why we're doing integrated delivery systems.
Maybe the AHA is right. Maybe once we move more fully into the wonderland of value-based payment arrangements everything will work out: better quality for same or lower costs. The American Medical Group Association (AMGA), the long-time trade association for physician groups, similarly says that their vision is:
I've lived through DRGs, RBRVS, capitation, global capitation, staff model HMOs, IPAs, and an array of cost/quality incentive programs -- each of which was supposed to be the next magic bullet -- so I'm not holding my breath that payors will finally be able to outsmart providers when it comes to controlling revenue.
Don't get me wrong: I've long been a believer both in large physician groups and in clinical integration between physicians and institutional care. But I worry that those strategies to improve health care delivery are now being more used more as tactics to maintain and even improve revenue. Heck, we don't seem to be able to get physicians to stop providing services even they admit are "low-value," as the Choosing Wisely initiative has tried to do.
As I've written before, when you have to create a new model that is supposed to be patient-centered (e.g., PCMH), and providers demand to get paid more just for participating it in, it's a pretty clear indication that our health care system isn't about patients but rather is about the providers.
The problem isn't the structures themselves but rather their focus.
Take physician groups. The death of the independent physician practice, working solo or in a small practice, has long been predicted (and nostalgically lamented). Honestly: would you rather be treated by a doctor practicing alone, or by one at the Mayo Clinic? Physician groups allow for things like development of best practices, administrative efficiencies, and, in this era of Big Data, larger data sets that can be used to improve patient care. When it comes to physician groups, bigger would seem to be better.
If physician groups are good, the theory goes, then integrating them clinically and financially with hospitals, such as through partnerships or common ownership, should even better. That allows for more aligned incentives and better coordination across the continuum of care. Everyone loves Kaiser-Permanente, right?
The AMA says solo practice physicians now are only 17% of all physicians, down from 40% in 1983, and that physician ownership of their practice has declined from 76% in 1983 to just over 50% now (although other surveys say as few as 35% of physicians described themselves as independent practice owners, down from 62% as recently as 2008). Our health care system, it would seem, is destined to be made up of large physician groups, many of which will be owned by hospitals.
Too bad both larger groups and hospital ownership apparently end up costing us more.
A new study in Health Affairs found that as physicians concentrate in larger groups, prices tend to go up, at least for the 15 high volume, high cost procedures the authors looked at. Twelve of the 15 procedures had prices that were 8 to 26 percent higher in areas with the highest physician concentrations; they found no significant relationship for the remaining three.
It might seem that whatever savings might be gained by becoming part of a group are not being passed on to consumers (or their health plans), and/or larger size allows groups to bargain for better reimbursement rates from payors.
An earlier survey, by one of the lead authors of the new study, found that more competition among physicians did, in fact, result in lower prices, at least for office visits. One might conclude that more concentration into larger physician practices may have less to do with greater efficiency or higher quality than it does with reducing competition.
The moral appears to be, if you don't want to compete with them, join them!
Then there is the hospital ownership effect. A study in JAMA Internal Medicine found that increased hospital/physician financial integration led to greater spending, primarily in outpatient care and almost entirely due to higher prices, not higher utilization. Again, the price increases are attributed to greater bargaining power. As one of the authors told The Wall Street Journal: "The market power that is in the hospital’s hands is conferred to the physician practice."
The AHA protests that the study "is not reflective of the changes happening in today’s health-care market," citing newer value-based payment arrangements and hospital price increases that are at historically low levels. That's kind of like saying, well, we weren't taking advantage of you before, but -- trust us -- in the future we really won't take advantage of you.
One visible impact of hospital ownership on physicians is the infamous facility fee add-on. You've been going to the same doctor for years, then the practice gets bought by a hospital, and the next time you go your bill suddenly has this "facility fee" added onto it. Same services, same office, same doctor -- but more expensive.
A good example of this practice is in Pittsburgh, where Highmark unilaterally decided to stop paying such fees for chemotherapy done at UPMC-owned oncologists' offices. Highmark says the fees are "irrational." UPMC says they are not only necessary but standard practice, including at Highmark's own hospital system, Allegheny Health. The matter is in court.
These kinds of fees, based on "place of service," are expressly permitted by Medicare, although one has to assume that they were not the intent of those rules. Of course the AHA defends them, saying that hospital-owned practices can bill as an outpatient facility because they are subject to the more onerous requirements that other hospital outpatient services are, but they just don't pass the sniff test. That's not supposed to be why we're doing integrated delivery systems.
Maybe the AHA is right. Maybe once we move more fully into the wonderland of value-based payment arrangements everything will work out: better quality for same or lower costs. The American Medical Group Association (AMGA), the long-time trade association for physician groups, similarly says that their vision is:
"Dramatically improved population health and care for patients at lower overall costs will be achieved by high-performing and clinically integrated medical groups and health systems."They've got all the right buzzwords (except they missed "value-based"), but AMGA has been around for 65 years, so where is that "dramatically improved" health and where are those lower costs?
I've lived through DRGs, RBRVS, capitation, global capitation, staff model HMOs, IPAs, and an array of cost/quality incentive programs -- each of which was supposed to be the next magic bullet -- so I'm not holding my breath that payors will finally be able to outsmart providers when it comes to controlling revenue.
Don't get me wrong: I've long been a believer both in large physician groups and in clinical integration between physicians and institutional care. But I worry that those strategies to improve health care delivery are now being more used more as tactics to maintain and even improve revenue. Heck, we don't seem to be able to get physicians to stop providing services even they admit are "low-value," as the Choosing Wisely initiative has tried to do.
As I've written before, when you have to create a new model that is supposed to be patient-centered (e.g., PCMH), and providers demand to get paid more just for participating it in, it's a pretty clear indication that our health care system isn't about patients but rather is about the providers.
The problem isn't the structures themselves but rather their focus.
Wednesday, October 14, 2015
The Grass Is Always Greener
Reuters reports that more hospitals are interested in having their own health plan, citing a 2014 survey by The Advisory Board that found one-third of 45 large health systems already had a health plan, with three-quarters of the rest already planning one or seriously considering it. A new report from Moody's predicts the same trend.
As the saying goes, be careful what you wish for, else you may get it.
Part of this trend is out of concern about the proposed mergers by mega-health plans like Aetna/Humana and Anthem/Cigna. Both the AMA and AHA have voiced their strong opposition to these mergers, citing anti-trust concerns (they were, of course, silent about the intra-market consolidation going on among health systems). Evidently many health care systems figure that the best way to fight an 800 pound gorilla is to have your own monkey.
In some ways, the time has never been better for health systems to have a health plan. Such plans typically operate in a single market, which is often a barrier for employer coverage. ACA has made individual coverage a hot market, with close to 10 million people receiving coverage through the exchanges, so operating only in single markets is less of a barrier.
Similarly, prior to ACA the trend in health plan networks had been wider networks, but under ACA that trend has been markedly reversed. According to McKinsey, almost half of exchange plans have narrow networks, and the percentage is higher in larger cities. Health system-specific health plans should fit in with this trend very well.
Health systems love to cite examples of integrated delivery/financing systems like Kaiser, Geisinger, Group Health Cooperative, Intermountain Healthcare, or UPMC. Yes, there are examples of health systems that offer successful health plans. No, that doesn't mean it is easy to do. Geisinger spun-off a consulting company, xG Health Solutions, to help other health systems become more like them, and UPMC did something similar with Evolent Health. Still, the other successes have been slow in coming.
As I've written before, several of those models have been around for decades. If they were bending the cost curve by even 1 percentage point a year, by now they should be 15%, 25%, even 50% lower in cost than their competitors. They are not. If the models were easily replicated, one would expect to find that they'd already spread widely. They have not. For the most part, they've stayed in their home markets; even Kaiser has struggled outside California.
It's not as easy as it looks, and it doesn't look all that easy.
As Moody's warns: "Not-for-profit hospitals with a health insurance business (often known as an integrated delivery system, or IDS) tend to operate at noticeably lower operating cash flow margins than similar health systems without insurance."
As if that wasn't cautionary enough, there's the example of the health insurance coops created by ACA to compete with the traditional health insurers. The largest coop, Health Republic Insurance of New York, is being shut down, despite their having gained over 200,000 members. The Kentucky Health Cooperative also recently announced it was closing. Coops in Iowa, Louisiana, Nevada, and Tennessee have also closed,
Indeed, this past July the HHS Office of Inspector General found that 21 of the 23 coops lost money in 2014, due in part that 13 of them had "significantly" lower enrollment than expected. Ray Herschman, president of xG Health Solutions, told Reuters that new health plans needed to aim at enrollment of at least 100,000, so the coop enrollment struggles should be particularly concerning to health systems.
The Kentucky Coop in particular blamed the failure of the federal risk corridor program, designed to cover higher-than-expected losses in the early years of the exchanges. HHS recently announced it is only granting about 13% of the almost $3b in payments requested by health plans. That's not HHS just being stingy; rather, it means that fewer health plans did better than expected and thus were able to "fund" the corridor. Even health plans with significant experience and market share had trouble making money in the exchanges.
This is not an easy business in which to start-up.
Even assuming health systems are comfortable with the financial risk of having a health plan, there are some other factors to consider:
As the saying goes, be careful what you wish for, else you may get it.
Part of this trend is out of concern about the proposed mergers by mega-health plans like Aetna/Humana and Anthem/Cigna. Both the AMA and AHA have voiced their strong opposition to these mergers, citing anti-trust concerns (they were, of course, silent about the intra-market consolidation going on among health systems). Evidently many health care systems figure that the best way to fight an 800 pound gorilla is to have your own monkey.
In some ways, the time has never been better for health systems to have a health plan. Such plans typically operate in a single market, which is often a barrier for employer coverage. ACA has made individual coverage a hot market, with close to 10 million people receiving coverage through the exchanges, so operating only in single markets is less of a barrier.
Similarly, prior to ACA the trend in health plan networks had been wider networks, but under ACA that trend has been markedly reversed. According to McKinsey, almost half of exchange plans have narrow networks, and the percentage is higher in larger cities. Health system-specific health plans should fit in with this trend very well.
Health systems love to cite examples of integrated delivery/financing systems like Kaiser, Geisinger, Group Health Cooperative, Intermountain Healthcare, or UPMC. Yes, there are examples of health systems that offer successful health plans. No, that doesn't mean it is easy to do. Geisinger spun-off a consulting company, xG Health Solutions, to help other health systems become more like them, and UPMC did something similar with Evolent Health. Still, the other successes have been slow in coming.
As I've written before, several of those models have been around for decades. If they were bending the cost curve by even 1 percentage point a year, by now they should be 15%, 25%, even 50% lower in cost than their competitors. They are not. If the models were easily replicated, one would expect to find that they'd already spread widely. They have not. For the most part, they've stayed in their home markets; even Kaiser has struggled outside California.
It's not as easy as it looks, and it doesn't look all that easy.
As Moody's warns: "Not-for-profit hospitals with a health insurance business (often known as an integrated delivery system, or IDS) tend to operate at noticeably lower operating cash flow margins than similar health systems without insurance."
As if that wasn't cautionary enough, there's the example of the health insurance coops created by ACA to compete with the traditional health insurers. The largest coop, Health Republic Insurance of New York, is being shut down, despite their having gained over 200,000 members. The Kentucky Health Cooperative also recently announced it was closing. Coops in Iowa, Louisiana, Nevada, and Tennessee have also closed,
Indeed, this past July the HHS Office of Inspector General found that 21 of the 23 coops lost money in 2014, due in part that 13 of them had "significantly" lower enrollment than expected. Ray Herschman, president of xG Health Solutions, told Reuters that new health plans needed to aim at enrollment of at least 100,000, so the coop enrollment struggles should be particularly concerning to health systems.
The Kentucky Coop in particular blamed the failure of the federal risk corridor program, designed to cover higher-than-expected losses in the early years of the exchanges. HHS recently announced it is only granting about 13% of the almost $3b in payments requested by health plans. That's not HHS just being stingy; rather, it means that fewer health plans did better than expected and thus were able to "fund" the corridor. Even health plans with significant experience and market share had trouble making money in the exchanges.
This is not an easy business in which to start-up.
Even assuming health systems are comfortable with the financial risk of having a health plan, there are some other factors to consider:
- Brand: Consumer ratings for health care providers are dipping, but health plans would love to have the kind of ratings providers get. Fairly or not, health plans get blamed for what they don't pay. That kind of negative perception could harm a health system's overall brand.
- Marketing: Health systems have tried to broaden their appeal to younger and healthier consumers, but still love to tout their expertise with serious conditions. That can lead to a risk selection disaster for a health plan.
- Regulation: Health systems certainly have plenty of regulation, but they may be surprised by the degree and types of regulations that health insurance brings. And they are not usually from the regulators health systems are used to. It is a big compliance leap.
- Customer service: If health systems think they get a lot of calls now, it's nothing like what they can expect with a health plan. Likely, more irate calls too. Customer service can be outsourced, of course, but that puts both customer contact and customer satisfaction in the hands of other entities.
- Focus: Both health plans and health systems are edging closer to population health management and coordination across the continuum of care, but the simple truth is that health insurance is not the same as providing health services. Health systems need to be comfortable that a having health plan aids in their focus rather than distracts from it. Does a health system CEO really want to add claims backlogs to the list of worries?
As Moody's said: "Different management expertise is needed to operate a commercial health insurance business versus an acute care hospital."
If a health system asked my opinion, I'd tell them to forget about developing a health plan. Instead, I'd recommend they focus on taking more risk via value-based payments, bundled payments, even global or semi-global payments as in an ACO. They'd learn about managing populations and dealing with upside/downside risks, without getting dragged all the way into the morass that having a health plan could bring.
Instead of coveting the what they perceive as the greener grass of health plans, perhaps health systems should, as Voltaire suggested, cultivate their own garden.
Thursday, October 8, 2015
Betting on the Future(s)
Pundits worry about the chilling effect that medical school debt -- which approaches $200,000, according to the AAMC -- has on our future physician workforce. If so, I'm wondering if health care should take a page out of a tactic being used for pro athletes: allow investors to buy shares of physicians' future income.
The company doing this for athletes is Fantex, It was launched in 2013 to some fanfare, particularly when their initial athlete IPO was to be for running back Adrian Foster. Foster signed away 20% of his future income for $10 million upfront. Investors could buy into the revenue stream for as little as $10 a share (sadly, the deal was postponed due to an injury). Fantex has gone on to sign something like nine NFL athletes and has now broken into MLB with the recent signing of Andrew Heaney.
Foster aside, most of the athletes whose shares are sold on Fantex are not the biggest names in their sports. They tend to be lower-tier athletes who still may expect to make several million dollars during their pro career but not so much that they don't find the the assurance of the upfront cash attractive. E.g., not so much the first pick in the NFL draft as the late first round or second round picks.
Fantex is looking to branch out to more sports, perhaps even to celebrities.
If you are going to be an orthopedic surgeon or a cardiovascular surgeon, which tend to be highly paid, you might not be interested, but if you are going into pediatrics or family medicine, you might see some appeal in such a deal.
While some investment experts are critical of Fantex, it's not a such crazy idea. FinTech darling SoFi is doing quite well focusing on refinancing debts for graduates of universities with a proven track record of high income alumni (think Harvard or Stanford). Medical school graduates are one of their prime targets, repackaging the loans and selling them.
The market must like their approach; SoFi has a $4b valuation after only 4 years of existence, and has been profitable for the past couple years. Making loan decisions based on expected future incomes of people and professions who tend to do very well financially seems like a pretty safe bet.
Would buying a share of that future income itself really be much different than, essentially, buying a share in the repayment of their medical school loans?
It's not that I'm all that concerned about medical school loans. Yes, they end up being a lot of money, but so does an undergraduate degree from, say, Notre Dame, or opting for an MBA or a law degree, for that matter. Financial institutions, even traditional ones instead of upstarts like SoFi, are usually quite happy to lend budding to new physicians to cover such debts.
And the real cost of becoming a doctor may not, in fact, be the cost of medical school but the "opportunity costs" of all that medical training, which has been estimated as being close to $800,000. The indentured servitude that medical school graduates must go through before being allowed to practice on their own (which is, I believe, unique to health care) accounts for the biggest part of these costs.
But I digress (and I've hit on the follies of our medical education system previously).
To be honest, I'm not even really all that interested in securitizing physicians' incomes, even for those (relatively) poor primary care physicians. Complaints about incomes aside, most physicians do quite well financially and, of course, much better than in most other countries. What I'm interested in is having the data on physicians that such an approach would require.
After all, you wouldn't (I hope) buy a stock or a mutual fund without some idea about how well it has performed and how well it is expected to do in the future. Not just stocks or mutual funds in general, but the specific ones you are interested in. And the same would presumably be true with a Fantex approach to health care; we'd be willing to invest in a specific physician but only if we could see some meaningful data on performance or expected performance of them.
And that, my friends, would be a game changer in health care.
We talk and talk and talk about transparency and pay-for-performance, but try finding out how many knee surgeries your would-be orthopedic surgeon has done, much less how many of those patients are happy with their surgery. Or how many are dead. And those would be easier to quantify than many other specialties we'd also be interested in.
I keep going back to something a colleague of mine said a few years ago: we can get more performance data on virtually any pro athlete than we can about any physician. That is crazy. He further proposed -- joking, I think -- that what we need are fantasy leagues for health care. I read with amazement about the hyper-growth of sports fantasy leagues, and wonder why we spend so time and energy on statistics for an activity that at most impacts our psychological health, but passively accept a dearth of comparable data on something that directly impacts our actual health.
The recent "insider trading" scandal at FanDuel and Draftkings, two leading fantasy sports companies, might seem like a cautionary note for trying anything remotely comparable in health care, but I'd say, on the contrary. We already have our own version of insider trading. Ask any doctor or nurse in a hospital which doctors they'd use, or stay away from, and they can tell you. They just don't.
We need to level the playing field. We need to see data on who is good, who is bad, and who is in-between. The efforts we've been doing to date -- e.g., Medicare's Physician Compare -- are well intended, but no sports fan would accept such paltry data for their fantasy choices.
We need to get people to be as passionate about their health as they are about their favorite sports.
Ironically, putting economic incentives like investments in, or fantasy "betting" on, individual physicians might just be our best hope.
The company doing this for athletes is Fantex, It was launched in 2013 to some fanfare, particularly when their initial athlete IPO was to be for running back Adrian Foster. Foster signed away 20% of his future income for $10 million upfront. Investors could buy into the revenue stream for as little as $10 a share (sadly, the deal was postponed due to an injury). Fantex has gone on to sign something like nine NFL athletes and has now broken into MLB with the recent signing of Andrew Heaney.
Foster aside, most of the athletes whose shares are sold on Fantex are not the biggest names in their sports. They tend to be lower-tier athletes who still may expect to make several million dollars during their pro career but not so much that they don't find the the assurance of the upfront cash attractive. E.g., not so much the first pick in the NFL draft as the late first round or second round picks.
Fantex is looking to branch out to more sports, perhaps even to celebrities.
If you are going to be an orthopedic surgeon or a cardiovascular surgeon, which tend to be highly paid, you might not be interested, but if you are going into pediatrics or family medicine, you might see some appeal in such a deal.
While some investment experts are critical of Fantex, it's not a such crazy idea. FinTech darling SoFi is doing quite well focusing on refinancing debts for graduates of universities with a proven track record of high income alumni (think Harvard or Stanford). Medical school graduates are one of their prime targets, repackaging the loans and selling them.
The market must like their approach; SoFi has a $4b valuation after only 4 years of existence, and has been profitable for the past couple years. Making loan decisions based on expected future incomes of people and professions who tend to do very well financially seems like a pretty safe bet.
Would buying a share of that future income itself really be much different than, essentially, buying a share in the repayment of their medical school loans?
It's not that I'm all that concerned about medical school loans. Yes, they end up being a lot of money, but so does an undergraduate degree from, say, Notre Dame, or opting for an MBA or a law degree, for that matter. Financial institutions, even traditional ones instead of upstarts like SoFi, are usually quite happy to lend budding to new physicians to cover such debts.
And the real cost of becoming a doctor may not, in fact, be the cost of medical school but the "opportunity costs" of all that medical training, which has been estimated as being close to $800,000. The indentured servitude that medical school graduates must go through before being allowed to practice on their own (which is, I believe, unique to health care) accounts for the biggest part of these costs.
But I digress (and I've hit on the follies of our medical education system previously).
To be honest, I'm not even really all that interested in securitizing physicians' incomes, even for those (relatively) poor primary care physicians. Complaints about incomes aside, most physicians do quite well financially and, of course, much better than in most other countries. What I'm interested in is having the data on physicians that such an approach would require.
After all, you wouldn't (I hope) buy a stock or a mutual fund without some idea about how well it has performed and how well it is expected to do in the future. Not just stocks or mutual funds in general, but the specific ones you are interested in. And the same would presumably be true with a Fantex approach to health care; we'd be willing to invest in a specific physician but only if we could see some meaningful data on performance or expected performance of them.
And that, my friends, would be a game changer in health care.
We talk and talk and talk about transparency and pay-for-performance, but try finding out how many knee surgeries your would-be orthopedic surgeon has done, much less how many of those patients are happy with their surgery. Or how many are dead. And those would be easier to quantify than many other specialties we'd also be interested in.
I keep going back to something a colleague of mine said a few years ago: we can get more performance data on virtually any pro athlete than we can about any physician. That is crazy. He further proposed -- joking, I think -- that what we need are fantasy leagues for health care. I read with amazement about the hyper-growth of sports fantasy leagues, and wonder why we spend so time and energy on statistics for an activity that at most impacts our psychological health, but passively accept a dearth of comparable data on something that directly impacts our actual health.
The recent "insider trading" scandal at FanDuel and Draftkings, two leading fantasy sports companies, might seem like a cautionary note for trying anything remotely comparable in health care, but I'd say, on the contrary. We already have our own version of insider trading. Ask any doctor or nurse in a hospital which doctors they'd use, or stay away from, and they can tell you. They just don't.
We need to level the playing field. We need to see data on who is good, who is bad, and who is in-between. The efforts we've been doing to date -- e.g., Medicare's Physician Compare -- are well intended, but no sports fan would accept such paltry data for their fantasy choices.
We need to get people to be as passionate about their health as they are about their favorite sports.
Ironically, putting economic incentives like investments in, or fantasy "betting" on, individual physicians might just be our best hope.
Tuesday, September 29, 2015
To ER Is Human
One of my favorite quotes from The Princess Bride is when Inigo Montoya tells Vizzini, who repeatedly uses the word "inconceivable" for situations that were not only conceivable but actually happening: "You keep using that word. I do not think it means what you think it means." I think of that line whenever I think about the use of "emergency" as part of "emergency rooms" (excuse me, they like to be called "emergency departments" now).
I was prompted to think of ERs by a WSJ op-ed by Dr. Paul Auerbach. In it, he argues that non-emergency visits to the ER aren't going to stop, much as we might wish patients to do a better job of evaluating when they are actually suffering an "emergency." He notes the limited access to timely care from primary care physicians, and how it is not reasonable to expect people to make such rational evaluations when they or their loved ones are suffering.
As he says, "You can't teach patients economics lessons when they don't feel well."
Dr. Auerbach wants more resources to "make emergency departments more efficient," as well as to build primary care and specialty capacity. ERs certainly could be more efficient, but I suspect that simply adding more physician capacity won't really get at the underlying problems. I do agree that these non-emergency visits are likely to continue, and that the health care system has to accommodate them, rather than making patients accommodate to it.
The rise of urgent care centers and retail clinics should be helping decrease ER visits, but neither those nor more people having coverage seem to be denting ER visits, which nearly half of us make every year.
According to the CDC, 27% of ER visits only had a 15 minute wait to see a doctor, nurse practitioner, or physician assistant, but third waited over an hour. Only 12% of visits lasted under an hour; the plurality (35%) lasted 2-3 hours. To Dr. Auerbach's point, less than 12% of all visits were evaluated as actually being "immediate" or "emergent."
Promedica has teamed with Yelp to give ER statistics by hospital, such as average ER wait times and average time before being sent home, more available to consumers (see Promedica's tool), hoping they'll check it before rushing off to the local ER, but they should be mindful of what Dr. Becker said about when to give economics lessons.
Making this data available may not have the impact Promedica/Yelp hope. Digital design/strategy firm Huge did a "neuromarketing" study on what impact posting average wait times had on consumers. They found that proximity was still paramount, regardless of expected wait times, but that posting the wait times could positively impact the perceived brand image of a hospital, even if their average wait was longer than the national average. Indeed, some thought shorter wait times meant worse quality.
What ERs tend to have in common is that many people are shocked at the cost. A 2013 study found wide variability in ER charges for common conditions, with the median charge of $1,233 being 40% higher than the average American pays in monthly rent. And good luck trying to find out the costs in advance.
We're making it too hard for consumers. We give them all these options -- not just ERs but free-standing ERs, not just urgent care centers but also retail clinics, plus physician offices, outpatient clinics, telehealth, even telehealth kiosks -- but aren't as good about helping them know when to use which. Widely touted app iTriage has the right idea -- steering users to the right providers/facilities based on their symptoms -- yet its recommendations always seem to include ERs anyway.
Honestly, if you are clear when which patients should go to which option for what conditions, you're smarter than I am. You probably are anyway, but what worries me is that I'm not sure many providers know either, even when a single health system is offering the options.
These efforts are good starts, but they're just scratching the surface of what needs to be done. Ideally, what we need is something like this:
I was prompted to think of ERs by a WSJ op-ed by Dr. Paul Auerbach. In it, he argues that non-emergency visits to the ER aren't going to stop, much as we might wish patients to do a better job of evaluating when they are actually suffering an "emergency." He notes the limited access to timely care from primary care physicians, and how it is not reasonable to expect people to make such rational evaluations when they or their loved ones are suffering.
As he says, "You can't teach patients economics lessons when they don't feel well."
Dr. Auerbach wants more resources to "make emergency departments more efficient," as well as to build primary care and specialty capacity. ERs certainly could be more efficient, but I suspect that simply adding more physician capacity won't really get at the underlying problems. I do agree that these non-emergency visits are likely to continue, and that the health care system has to accommodate them, rather than making patients accommodate to it.
The rise of urgent care centers and retail clinics should be helping decrease ER visits, but neither those nor more people having coverage seem to be denting ER visits, which nearly half of us make every year.
According to the CDC, 27% of ER visits only had a 15 minute wait to see a doctor, nurse practitioner, or physician assistant, but third waited over an hour. Only 12% of visits lasted under an hour; the plurality (35%) lasted 2-3 hours. To Dr. Auerbach's point, less than 12% of all visits were evaluated as actually being "immediate" or "emergent."
Promedica has teamed with Yelp to give ER statistics by hospital, such as average ER wait times and average time before being sent home, more available to consumers (see Promedica's tool), hoping they'll check it before rushing off to the local ER, but they should be mindful of what Dr. Becker said about when to give economics lessons.
Making this data available may not have the impact Promedica/Yelp hope. Digital design/strategy firm Huge did a "neuromarketing" study on what impact posting average wait times had on consumers. They found that proximity was still paramount, regardless of expected wait times, but that posting the wait times could positively impact the perceived brand image of a hospital, even if their average wait was longer than the national average. Indeed, some thought shorter wait times meant worse quality.
What ERs tend to have in common is that many people are shocked at the cost. A 2013 study found wide variability in ER charges for common conditions, with the median charge of $1,233 being 40% higher than the average American pays in monthly rent. And good luck trying to find out the costs in advance.
We're making it too hard for consumers. We give them all these options -- not just ERs but free-standing ERs, not just urgent care centers but also retail clinics, plus physician offices, outpatient clinics, telehealth, even telehealth kiosks -- but aren't as good about helping them know when to use which. Widely touted app iTriage has the right idea -- steering users to the right providers/facilities based on their symptoms -- yet its recommendations always seem to include ERs anyway.
Honestly, if you are clear when which patients should go to which option for what conditions, you're smarter than I am. You probably are anyway, but what worries me is that I'm not sure many providers know either, even when a single health system is offering the options.
Some ERs have created separate triage tracks with distinct pricing and waits for different levels of need. Others are using technology to accomplish that. Houston has launched ETHAN -- Emergency Tele-health and Navigation -- for its 911 EMTs. If EMTs believe a 911 caller doesn't actually have an emergency, the EMTs at the scene can do a video consult with an emergency physician, who can then steer the patient to other options if appropriate, such as at primary care clinics.
Similarly, Jefferson Hospital in Philadelphia uses their JeffConnect telehealth service to connect potential ER visitors to do a video consult with an ER doctor, expecting they can deter some visits. The service costs $49 per visit -- much cheaper than an ER visit would be.
These efforts are good starts, but they're just scratching the surface of what needs to be done. Ideally, what we need is something like this:
- A service -- web-based, app, and/or phone -- lets you explain your health issue, and uses algorithms/AI to help identify the suspected problems(s).
- Depending on what is wrong, it might automatically call 911, call Uber to get you to the ER with the shortest wait time/shortest distance/most expertise with your problem, or connect you to a physician via video consult for further evaluation.
- If the problem is not truly an emergency, it can steer you to lower cost, shorter wait options, perhaps the next day, possibly making an appointment for you.
- The service would keep your health history, current prescriptions, and insurance information, then transmit those, your self-described symptoms and proposed diagnosis to whichever provider you are sent to, so you don't have to start all over again when you arrive.
None of that is beyond our current technological capabilities...so why doesn't such a service exist?
Patients are still going to end up in the "wrong" place, but we can help make that happen less often, and we can try to stop penalizing them -- through higher costs, longer waits, and unnecessary tests -- when they do. It's supposed to be patient-centered, not ER-centered, right?
Tuesday, September 22, 2015
Can Slick Trump Sick?
Health insurance is getting some love from investors, and not only the money going to the increasing consolidation of the industry giants. CB Insights says $1.4b of venture capital has gone to the insurance tech space since the beginning of 2014, with health insurance-related investments getting more than all other insurance sectors combined.
A lot of that money is going to companies that make it easier to deal with health insurance, but some is going to start-ups -- like Oscar, Clover Health, and Zoom+ -- that actually hope to reinvent the nitty-gritty, often grimy business of providing health insurance (or, as Wired put it, at least make it "suck less").
As some of the health co-ops are finding, though, it's not so easy to break into health insurance.
Oscar, of course, has long been a media darling. Last April they raised $145 million in a funding round that effectively valued them at $1.5b, and Google just put in another $32 million that ups that valuation to $1.75b. All this for a company that only has 40,000 members, is offered only in New York/New Jersey (with plans to expand to California and Texas), and which in 2014 lost $28 million on $57 million in revenue. But never mind all that; they've got a nice website.
That's not really fair, of course. They've focused on using technology to improve the customer experience, are ahead of the industry curve on use of technology like fitness trackers and telehealth, and are working to use data to match patients with the best physicians for their conditions. Still, as CEO Mario Schlosser admitted last year to Fortune, in wake of member complaints about ineffective communication as to how the health plan actually worked, "The healthcare system is astoundingly complex."
Oh, really?
Clover Health, which just raised $100 million in a funding round through some impressive lead investors, has a somewhat different strategy. It focuses on the Medicare population, putting their primary emphasis on using data to improve patient outcomes.
Clover uses their algorithms to identify high-risk patients, sends nurse practitioners to their homes to develop personalized care plans, and continually loops in new data to update patient profiles. The key is integrating data from disparate sources -- e.g., medical records, lab tests, even contacts with members -- to create an overall patient profile, then identify and fill any gaps.
As CEO Vivek Garipalli told TechCrunch, "You imagine a Medicare patient goes to a primary doctor’s office, goes to a cardiologist, goes to a hospital, there is no quarterback for that data. No one has the time or the data to guide that patient and coordinate all those interactions and make sure each provider gets the right info at the right time.” This is the elusive goal of interoperability and of patient-centered teams, but Clover thinks they've cracked that challenge.
So far Clover (headquartered in San Francisco) is only available in six New Jersey counties, but they claim to have 50% fewer hospital admissions and 34% fewer readmissions than the average for Medicare patients in those counties. Most of their competitors would claim to have similar efforts for high-risk patients, so we'll have to see if their model scales.
Then there is Zoom+, or, rather, "Zoom+ Performance Health Insurance." It is the outgrowth of ZoomCare, a network of retail clinics in Portland (OR). Zoom+ claims to be "the nation’s first health insurance system built from the ground up to enhance human performance," and thinks of itself as "Kaiser 4.0."
Hmm.
Zoom+ has focused heavily on the user experience, wanting "health care to be more like visiting an Apple store," according to Fast Company Design's profile of them. CEO Dave Sanders says: "Health care is one of the largest household spending categories other than a car or food. For that kind of investment, it needs to be a life-enhancing platform, not just a commodity or a utility. Oh, and by the way, when you’re really sick, it’s got your back too."
The five design principles that guide Zoom are:
A lot of that money is going to companies that make it easier to deal with health insurance, but some is going to start-ups -- like Oscar, Clover Health, and Zoom+ -- that actually hope to reinvent the nitty-gritty, often grimy business of providing health insurance (or, as Wired put it, at least make it "suck less").
As some of the health co-ops are finding, though, it's not so easy to break into health insurance.
Oscar, of course, has long been a media darling. Last April they raised $145 million in a funding round that effectively valued them at $1.5b, and Google just put in another $32 million that ups that valuation to $1.75b. All this for a company that only has 40,000 members, is offered only in New York/New Jersey (with plans to expand to California and Texas), and which in 2014 lost $28 million on $57 million in revenue. But never mind all that; they've got a nice website.
That's not really fair, of course. They've focused on using technology to improve the customer experience, are ahead of the industry curve on use of technology like fitness trackers and telehealth, and are working to use data to match patients with the best physicians for their conditions. Still, as CEO Mario Schlosser admitted last year to Fortune, in wake of member complaints about ineffective communication as to how the health plan actually worked, "The healthcare system is astoundingly complex."
Oh, really?
Clover Health, which just raised $100 million in a funding round through some impressive lead investors, has a somewhat different strategy. It focuses on the Medicare population, putting their primary emphasis on using data to improve patient outcomes.
Clover uses their algorithms to identify high-risk patients, sends nurse practitioners to their homes to develop personalized care plans, and continually loops in new data to update patient profiles. The key is integrating data from disparate sources -- e.g., medical records, lab tests, even contacts with members -- to create an overall patient profile, then identify and fill any gaps.
As CEO Vivek Garipalli told TechCrunch, "You imagine a Medicare patient goes to a primary doctor’s office, goes to a cardiologist, goes to a hospital, there is no quarterback for that data. No one has the time or the data to guide that patient and coordinate all those interactions and make sure each provider gets the right info at the right time.” This is the elusive goal of interoperability and of patient-centered teams, but Clover thinks they've cracked that challenge.
So far Clover (headquartered in San Francisco) is only available in six New Jersey counties, but they claim to have 50% fewer hospital admissions and 34% fewer readmissions than the average for Medicare patients in those counties. Most of their competitors would claim to have similar efforts for high-risk patients, so we'll have to see if their model scales.
Then there is Zoom+, or, rather, "Zoom+ Performance Health Insurance." It is the outgrowth of ZoomCare, a network of retail clinics in Portland (OR). Zoom+ claims to be "the nation’s first health insurance system built from the ground up to enhance human performance," and thinks of itself as "Kaiser 4.0."
Hmm.
Zoom+ has focused heavily on the user experience, wanting "health care to be more like visiting an Apple store," according to Fast Company Design's profile of them. CEO Dave Sanders says: "Health care is one of the largest household spending categories other than a car or food. For that kind of investment, it needs to be a life-enhancing platform, not just a commodity or a utility. Oh, and by the way, when you’re really sick, it’s got your back too."
The five design principles that guide Zoom are:
- Credibility begins with aesthetics
- Define "anti-requirements"
- Vertically integrate
- Build trust with savvy partnerships
- Accentuate the positive
By comparison, you don't get the feeling that, say, Anthem focuses a lot on aesthetics.
Zoom+ features not just cool retail centers but also mobile capabilities, a Personal Performance Path, and a Zoom+ Guru, among other services. It is not your mother's health insurance, and right now can't be yours either unless you happen to live in Portland.
I'm all for reinventing health insurance. I'm all for making the customer experience much, much better in health insurance and in health care generally. But I do worry that some of these upstarts may be taking advantage -- perhaps inadvertently -- of one of the underlying problems with health insurance: risk selection beats execution.
Here's why: About 5% of the population incurs about 50% of the overall costs. If the overall cost in a population is $6,000 per person, as it is for employer coverage, then those 5% average $60,000 each, while the remaining 95% average a little under $3,200. It doesn't take too much of a change in the make-up of a population to dramatically skew its costs:
Company A thus gets a 17% cost advantage over Company B if it can just slightly lower the percentage of the really sick people who enroll in it. That can offset a lot of administrative efficiencies, provider contracting advantages, or population health management efforts.
Of course, under ACA, health insurers can't overtly practice risk selection. They can't medically underwrite, can't cancel coverage, and have to take all-comers. They can't even blatantly market to healthy people. ACA also has provisions to risk adjust between health insurers, but they are at best imperfect.
Health insurers can, however, market features that are more likely to appeal to younger, healthier customers, like snazzy websites, fitness trackers, or training advice. None of those are only of interest to "healthy" people, but, as the chart above suggests, it doesn't take much of a shift in the risk profile to have noticeable impacts on costs.
Health insurance needs more consumer-focused technology, more effective use of data, and more focus on promoting health instead of reacting to sickness. However, I'm not getting too excited until I see a health insurer that does away with provider networks, refuses to be complicit in outlandish provider charges, and offers a plan of benefits that consumers can actually understand.
Until then, we may just be putting new colors on the old chassis.
Monday, September 14, 2015
Giving It Away
I'm fascinated with companies bold enough to blow up their own business model. I'm especially fascinated when part of how they do so by giving away services "for free." A couple weeks ago I wrote about how Microsoft was attempting to do both of those, and now Verizon is making an equally interesting move with their introduction of Go90.
As usual, I only wish the example was from a health care company.
Go90 is a streaming service that allows users to watch television shows, videos, and similar content on their mobile devices (the name reflects how users typically orient their mobile devices to watch videos in landscape mode). Unlike previous streaming services, such SlingTV or HBO NOW, the streaming is only for mobile devices, rather than Internet streaming more broadly (although Verizon may follow-up Go90 with a TV service). Plus, of course, it's "free," whereas SlingTV and HBO NOW both carry monthly fees.
Verizon acquired the platform for Go90 from Intel, which had been developing an Internet video service in its own effort to revamp its business, That service, named OnCue, fell out a favor within Intel after a CEO change, and Verizon snapped it up for under $200 million. The stakes for Verizon got higher after AT&T acquired DirecTV, which is AT&T's effort to stay relevant in a more interconnected world.
The cable industry is already undergoing upheaval, realizing that its traditional bundling of channels may no longer be viable. Various options have sprung up to let viewers have more control over which channels/programs they have to pay for (including Verizon's previously announced "skinny" package).
Even more significantly, the cable industry is terrified that they're losing the eyeballs of younger viewers, as illustrated by this graphic from The Wall Street Journal:
Verizon is trying to combat this trend by directly targeting millennials with Go90, using their favorite devices for watching media and at their favorite price point. In order to increase appeal to non-Verizon customers, they're not limiting it to Verizon customers, nor branding it Verizon, They further hope that Go90 will become "social entertainment," increasing its appeal to those uber-connected (pun intended) millennials.
Of course, "free" is rarely actually free. The service does include ads, and, as Variety reports, all that content counts towards data plans, which are not free. Still, if you were going to watch your videos on your phone/tablet anyway, a free service like Go90 should have some appeal.
The thing that struck me initially was the chart showing video patterns by age. It looks surprisingly similar to many charts of health care usage by age, such as the percentage of people with a primary care doctor by age (64% for 18-34 versus 90% for the 55+, according to The Physicians Foundation), or the number of physician visits by age, according to the CDC:
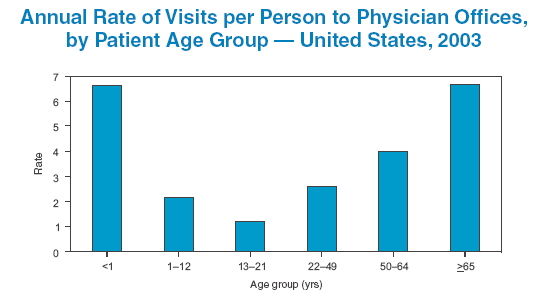
These patterns may not scare the health care industry the way that the corresponding video medium preferences scare the cable industry. After all, health care professionals can rationalize, as people get older they'll use more health care services, and, anyway, we seem to be developing chronic diseases at earlier and earlier ages (e.g., the recent study on diabetes/pre-diabetes prevalence), so the health care industry can always expect people to come to them.
Maybe. But maybe not; the future only resembles the past until it doesn't, and then it can look entirely different. I think health care should be placing a few more bets in case the younger population decides to ditch accessing care in traditional ways like they're ditching cable.
An obvious parallel to Go90 would be with telehealth. I keep reading about its explosive growth, but most of the uses still appear to be tied to health plans, with their deductibles, copays, and/or coinsurance. There are some direct-to-consumer offerings, such as through American Well or Doctors on Demand, but they typically charge per visit or per month.
It'd be interesting to see what would happen if a health system or physician group let people access all the virtual care they wanted "for free," while still charging for in-person services.
CVS recently announced it would be piloting services with three different telehealth companies, mostly in connection with its MinuteClinic offerings. CVS was the first to rid its stores of tobacco products, and it would be equally bold for them to offer a free telehealth service to customers. One would think the in-clinic/in-store referrals could more than pay for the service, and I'd bet that some health systems might pay for the right to be local referral centers for specialty care.
But we shouldn't only be thinking about free video services just because that is what Go90 happened to do. The underlying "problem" in reaching young people about health services is that, generally, they are more likely to be healthy -- or, at least, think they are healthy. Seeing a doctor, even virtually, is just not something they really want to do, unlike watching TV shows on their smartphones. If the health care industry wants to engage younger customers, it needs to do so for activities that they already want to do.
For example, pharmaceutical companies are already tapping Fitbits as a way to collect better data on people in clinical trials, and employer wellness programs have also jumped on the Fitbit bandwagon. Both of those are intriguing starts, but I doubt either group of users have any doubts about the reason for the largess. They only re-enforce the existing business models, rather than appear to upend them.
Similarly, there are already over a hundred thousand health-related apps, many of which have free versions, but not many of which threaten the existing health care business models. When we see apps that lets you, say, perform and interpret your own labs or imaging for "free," that would be revolutionary.
The interesting question will be whether someone in the health care industry will voluntarily up-end their own business model, as Verizon is doing with theirs, or if someone from outside the industry does it for them.
I know what my bet would be.
As usual, I only wish the example was from a health care company.
Go90 is a streaming service that allows users to watch television shows, videos, and similar content on their mobile devices (the name reflects how users typically orient their mobile devices to watch videos in landscape mode). Unlike previous streaming services, such SlingTV or HBO NOW, the streaming is only for mobile devices, rather than Internet streaming more broadly (although Verizon may follow-up Go90 with a TV service). Plus, of course, it's "free," whereas SlingTV and HBO NOW both carry monthly fees.
Verizon acquired the platform for Go90 from Intel, which had been developing an Internet video service in its own effort to revamp its business, That service, named OnCue, fell out a favor within Intel after a CEO change, and Verizon snapped it up for under $200 million. The stakes for Verizon got higher after AT&T acquired DirecTV, which is AT&T's effort to stay relevant in a more interconnected world.
The cable industry is already undergoing upheaval, realizing that its traditional bundling of channels may no longer be viable. Various options have sprung up to let viewers have more control over which channels/programs they have to pay for (including Verizon's previously announced "skinny" package).
Even more significantly, the cable industry is terrified that they're losing the eyeballs of younger viewers, as illustrated by this graphic from The Wall Street Journal:
Verizon is trying to combat this trend by directly targeting millennials with Go90, using their favorite devices for watching media and at their favorite price point. In order to increase appeal to non-Verizon customers, they're not limiting it to Verizon customers, nor branding it Verizon, They further hope that Go90 will become "social entertainment," increasing its appeal to those uber-connected (pun intended) millennials.
Of course, "free" is rarely actually free. The service does include ads, and, as Variety reports, all that content counts towards data plans, which are not free. Still, if you were going to watch your videos on your phone/tablet anyway, a free service like Go90 should have some appeal.
The thing that struck me initially was the chart showing video patterns by age. It looks surprisingly similar to many charts of health care usage by age, such as the percentage of people with a primary care doctor by age (64% for 18-34 versus 90% for the 55+, according to The Physicians Foundation), or the number of physician visits by age, according to the CDC:

These patterns may not scare the health care industry the way that the corresponding video medium preferences scare the cable industry. After all, health care professionals can rationalize, as people get older they'll use more health care services, and, anyway, we seem to be developing chronic diseases at earlier and earlier ages (e.g., the recent study on diabetes/pre-diabetes prevalence), so the health care industry can always expect people to come to them.
Maybe. But maybe not; the future only resembles the past until it doesn't, and then it can look entirely different. I think health care should be placing a few more bets in case the younger population decides to ditch accessing care in traditional ways like they're ditching cable.
An obvious parallel to Go90 would be with telehealth. I keep reading about its explosive growth, but most of the uses still appear to be tied to health plans, with their deductibles, copays, and/or coinsurance. There are some direct-to-consumer offerings, such as through American Well or Doctors on Demand, but they typically charge per visit or per month.
It'd be interesting to see what would happen if a health system or physician group let people access all the virtual care they wanted "for free," while still charging for in-person services.
CVS recently announced it would be piloting services with three different telehealth companies, mostly in connection with its MinuteClinic offerings. CVS was the first to rid its stores of tobacco products, and it would be equally bold for them to offer a free telehealth service to customers. One would think the in-clinic/in-store referrals could more than pay for the service, and I'd bet that some health systems might pay for the right to be local referral centers for specialty care.
But we shouldn't only be thinking about free video services just because that is what Go90 happened to do. The underlying "problem" in reaching young people about health services is that, generally, they are more likely to be healthy -- or, at least, think they are healthy. Seeing a doctor, even virtually, is just not something they really want to do, unlike watching TV shows on their smartphones. If the health care industry wants to engage younger customers, it needs to do so for activities that they already want to do.
For example, pharmaceutical companies are already tapping Fitbits as a way to collect better data on people in clinical trials, and employer wellness programs have also jumped on the Fitbit bandwagon. Both of those are intriguing starts, but I doubt either group of users have any doubts about the reason for the largess. They only re-enforce the existing business models, rather than appear to upend them.
Similarly, there are already over a hundred thousand health-related apps, many of which have free versions, but not many of which threaten the existing health care business models. When we see apps that lets you, say, perform and interpret your own labs or imaging for "free," that would be revolutionary.
The interesting question will be whether someone in the health care industry will voluntarily up-end their own business model, as Verizon is doing with theirs, or if someone from outside the industry does it for them.
I know what my bet would be.
Subscribe to:
Posts (Atom)

